Working for patients:
How improving the experience of patients with long-term conditions can deliver the Government’s ten year health plan

Executive summary
On his first day in office the Secretary of State for Health and Social Care, Wes Streeting labelled the NHS ‘broken but not beaten’.1 Whilst the NHS is undertaking record volumes of activity, there are long backlogs for treatment and patient satisfaction has fallen sharply.2 Streeting has been clear that the Government’s forthcoming Ten Year Health Plan to repair the system will be co-designed with the public, partner organisations and healthcare staff.3
Since last autumn the Government has run an extensive engagement exercise gathering feedback across these groups and many others. By the end of the exercise, the aim is to have had the biggest conversation on the future of the NHS ever held. At the heart of the plan are three shifts: moving care from hospital to community, shifting from sickness to prevention, and re-designing services from analogue to digital.
An ageing population and rises in multi-morbidity mean that 25 million people in England now have a long-term condition (LTC) such as blood pressure, diabetes, rheumatoid arthritis and back pain. Over the coming years this number is set to rise significantly.
This research argues that understanding the experience of people with LTCs needs to be at the heart of the Government’s plan. People with LTCs account for 70% of GP appointments and 50% of hospital activity.4
Understanding if these patients are feeling supported to manage their condition, able to access the care in the community they need, are avoiding complications with their condition, alongside their views on the usability and quality digital services, will be integral to assessing whether the three shifts are working in practice.
The experience of patients within the NHS is captured through a wide range of national and local surveys. But measuring and acting on the experience of patients has been de-prioritised in recent years with a far greater emphasis placed on improving access to services and waiting times for treatment. This is despite there being extensive evidence that improving patient experience can improve the quality of care and reduce more expensive healthcare use.5
The lack of prioritisation of patients with LTCs, which worsened during the COVID-19 pandemic and after, coupled with fragmented data collection methods and other structural challenges means the current system is not set-up for success.
This paper proposes a new nationally and locally blended policy model, based on the Core20PLUS5 health inequalities programme, to help embed the experience of patients with LTCs at the heart of delivering and monitoring the Government’s three policy shifts.6
To do so requires a four stage approach. Beginning with auditing what is currently being collected and using this to then inform and build a small number of more effective national experience measures aligned to the three shifts. It involves working with local systems to embed processes and support effective public and patient engagement alongside utilising new technologies to gather and analyse the feedback of patients and reporting back on progress.
In taking such actions the Government will be able to see whether the shifts in the Ten Year Plan are working for those with LTCs.
The latest NHS restructure, announced in March 2025, creates concerns that knowledge and expertise will flow out of the system in how patient experience is collected, analysed and acted upon.7 These fears are live and happening in real time as highlighted in National Voices’ recent report for the Health and Social Care Committee.8
De-prioritising patient experience at this point (framed as part of cuts to bureaucracy) would be completely counter-productive, not only for patients but for the Government itself.
Recording improvements in patient experience will support the Government’s aim of improving very low patient satisfaction rates – just one in five people say they are ‘satisfied’ with the way the NHS runs – bringing not only obvious direct patient but also political benefits.
Instead this restructure needs to be seen as an opportunity to finally embed patients and patient experience at the heart of the new health system.
This is an opportunity that must now be taken.
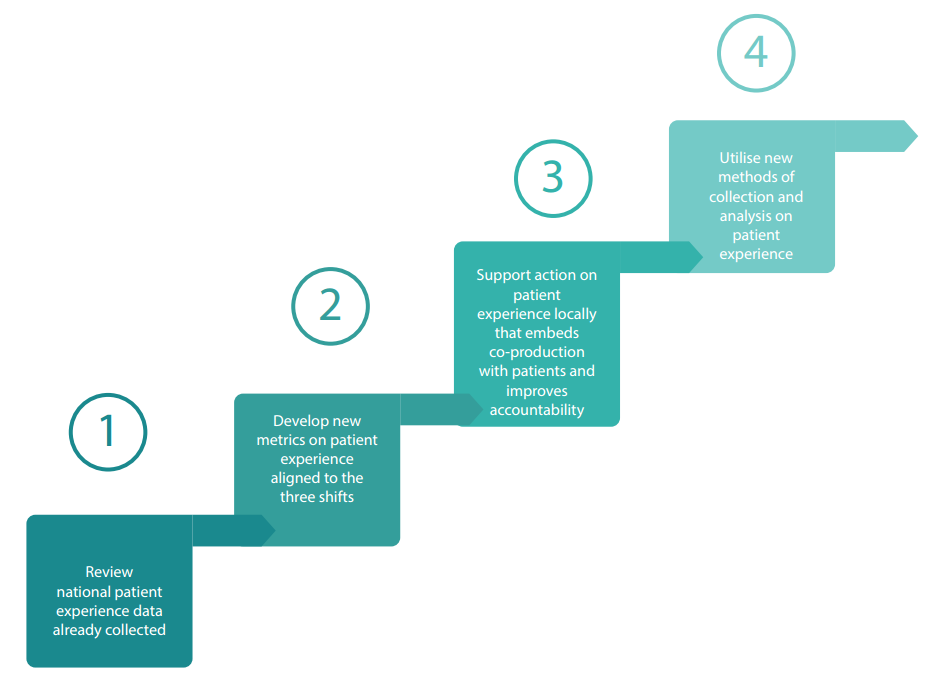
Action plan for change
This report proposes a four part action plan for prioritising and improving the experience of patients with LTCs within the NHS.
1 https://labour.org.uk/updates/press-releases/wes-streeting-speech-at-labour-party-conference-2024/
2 https://natcen.ac.uk/publications/public-attitudes-nhs-and-social-care
5 https://assets.publishing.service.gov.uk/media/5a7c3a5b40f0b67d0b11fbaf/7432.pdf
7 https://www.hsj.co.uk/integrated-care/revealed-the-icb-staff-targeted-for-redundancy/7039077.article
This report was funded by AbbVie; AbbVie had no influence on the content or editorial input of the report. Full editorial control sits with National Voices and Future Health Research.